INTRODUCTION
The temporomandibular joint (TMJ) is a complex lubrication joint between the mandibular fossa of the temporal bone and the articular process of the mandible. The TMJ consists of a synovial membrane, a joint pocket, a joint disc, and bone tissue. Unlike other synovial joints, the articular cartilage of the TMJ is characterized by a layer of connective tissue.1 The TMJ is one of the most used joints in the human body, and it moves more than 2,000 times a day. About 40–60% of the population has a TMJ disorder and has been reported to experience pain and limitation of the TMJ range of motion.2,3 Symptoms of TMJ disorders include a limited range of motion of the mandible, masticatory and joint pain, joint sounds (clicking, popping, or bone fricative sounds), fascia pain, and functional limitations.4 The most common symptoms of TMJ disorders are reportedly joint and muscle pain.5 TMJ disorders are caused by various and complex factors; the main factors are overactivity of the muscles and abnormal functional activities (e.g., incorrect biting) due to factors such as trauma, emotional stress, and malocclusion.3,6,7
The two TMJs are bilateral, and because both sides of the mandible roll or slide together, one TMJ cannot be moved without affecting the other. However, chewing food is often performed asymmetrically,8 and a study found that about 78% of the subjects preferred using one side during mastication.9 The position and movement of the TMJ is controlled by the masticatory muscles around the joint, including the masseter, temporalis, medial pterygoid, and lateral pterygoid. When biomechanical and physiological imbalance of these muscles occurs, TMJ disorders can be occurred.5,10
It has been reported that people with TMJ disorders have a high degree of asymmetry in the masticatory muscles.11 In the resting posture, the masseter has the highest asymmetry index compared to the digastric, anterior masseter, anterior temporalis, and sternocleidomastoid. The masseter thickness asymmetry in the resting position is a result of preferring to use one side of the mouth during mastication. Therefore, it is necessary to measure the masseter thickness asymmetry in the resting position to determine whether the asymmetry that appears in people with TMJ disorders is due to pain or muscle weakness.
People with TMJ disorders generally have a reduced mouth-opening range, making it difficult to perform the functional movement of putting food into the mouth.12 When they open their mouths and the TMJ exceeds the limited range, inflammation and pain occur. As a result, they restrict their mouth opening range to minimize pain.
The opening of the mouth involves a pure rotational movement until the incisors are 2.0–2.5 cm apart. After the rotation movement reaches its maximum, a translation movement occurs.3 In previous studies, tape measures have mainly been used to measure the range of motion of the mouth. However, this method has been shown to result in a measurement error of 0.2–0.3 cm, and the reliability is not high.13 Therefore, in this study, a motion capture device was used to measure rotational and translational movements during TMJ opening in subjects with and without TMJ dysfunction. The aim of this study was to compare the asymmetry of the rotation and translation distance and masseter thickness in subjects with and without TMJ pain.
METHODS
The study details were verbally shared with potential subjects before recruitment. All subjects expressed their willingness to participate, and verbal consent was obtained before subjects participated. This study was approved by the Baekseok University Human Studies Committee (BUIRB-202102-HR-043). A total of 15 subjects with TMJ pain made up the TMJ group, and 15 subjects without TMJ pain made up the control group. The subjects’ ages ranged from 20 to 26 years, and their average age was 23 years (Table 1). All subjects were classified into the TMJ group and the control group according to their answers to the following two questions.14 (1) Have you experienced pain in your temple, face, in front of the ears (TMJ), or jaw at least once within the past week? (2) Have you experienced jaw pain when opening your mouth or chewing food at least once within the past week? Those who answered “yes” to both questions were assigned to the TMJ group, and those who answered “no” to both questions were assigned to the control group. Exclusion criteria included neurological problems, receiving regular dental treatment, experience of trauma around the neck or jaw, and participation in the study.
| TMJ group (n=15) | Control group (n=15) | |
|---|---|---|
| Age (yr) | 23.2±1.3 | 22.8±2.2 |
| Height (cm) | 166.3±9.4 | 166.9±8.7 |
| Weight (kg) | 60.7±12 | 64.9±14.3 |
| Body mass index | 21.8±2.9 | 23.1±4 |
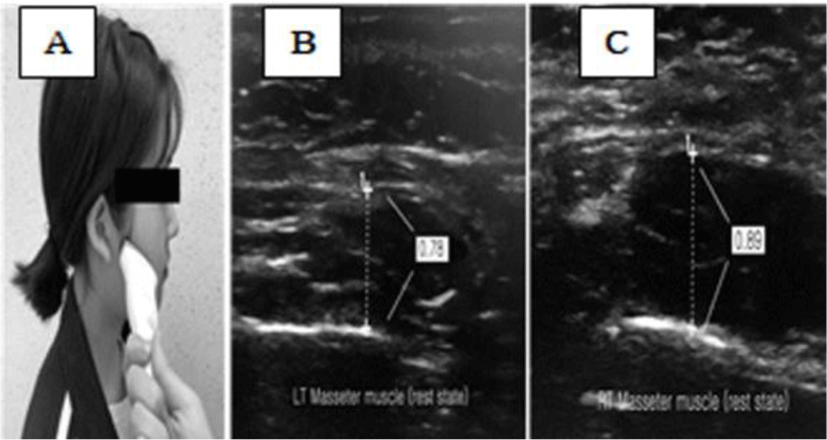
The LOGIQ P6 PRO (GE Inc., New Jersey, USA) was used to measure the masseter muscle thickness. The ultrasonic probe was placed at an angle of 60° to the skin surface 2.5 cm above the angle of the mandibular of the subject.15 Both masseter muscles were measured three times, and average values were calculated.
To measure the maximum mouth opening and rotation, the subject was placed on a chair with a backrest, and the distance between the camera (on a tripod) and the nose was fixed at 50 cm. Mouth opening was repeated three times to derive images using Image J software (Image Processing and Analysis in Java version 1.50i, USA, National Institutes of Health).
The subjects were placed in a sitting position. The examiner asked each subject to maintain a sitting posture with their head upright.15 Images of the left and right masseter muscles were collected with the subject’s mouth in a resting position, and a total of three images were saved. To rest the TMJ, the tongue was placed on the hard palate just behind the upper teeth, the upper and lower teeth were naturally spread apart, and the lips were closed and facing forward.17 The thickness of the masseter muscles was determined by drawing vertical lines on the muscles, excluding the fascia, in each image (Figure 1).
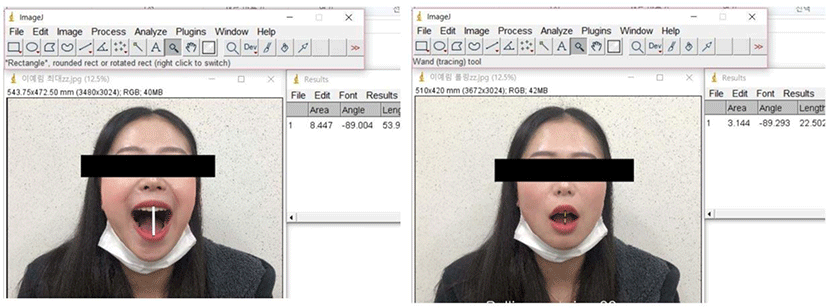
The maximum and rotation mouth opening were measured while the subject sat upright in a chair with a backrest and faced forward. To measure the maximum mouth opening, the mouth was opened as wide as possible, and the distance between the upper and lower teeth was measured. To measure the maximum mouth opening, the examiner asked the subject to “open your mouth as wide as you can”.
To measure the rotation mouth movement, the examiner asked the subject to “slowly open your mouth until I told them to stop”. The examiner palpated the subject’s both mandibular condyles with both hands and said “stop” before the condyles were translated forward, the distance between the upper and lower teeth was measured. When the maximum and rotation mouth opening were performed, Image J was used to take pictures of each subject and perform the measurements (Figure 2).
RESULTS
When the maximum and rotation mouth opening of the TMJ group and control group were compared, there was a significant difference between the TMJ group and the control group (p<0.05) (Table 2).
| TMJ group (n=15) | Control group (n=15) | p | |
|---|---|---|---|
| Maximum mouth opening (cm) | 45.47±2.36 | 49.27±3.02 | 0.011 |
| Rotation mouth opening (cm) | 23.80±2.08 | 34.13±3.06 | 0.012 |
The results showed that there was no significant difference in masseter thickness between the TMJ group and the control group (Table 3).
| TMJ group (n=15) | Control group (n=15) | p | |
|---|---|---|---|
| Masseter asymmetry index* | 0.98 | 1.06 | 0.447 |
DISCUSSION
Temporomandibular disorders (TMD) are the most common pain syndromes in the oral and maxillofacial regions and may be associated with the bilateral TMJ, the mastication muscles, and the blood vessels and nerves distributed in these tissues. The major symptoms of TMD include masticatory muscle and TMJ pain, TMJ sounds, and restriction of mandibular movement, and related symptoms include ear pain, stiffness, tinnitus, dizziness, neck pain, and headache.18,19,20 The frequency of pain in the TMJ tends to increase with modern people’s exposure to poor eating habits, lifestyle changes, and social and psychological problems.
The purpose of this study was to investigate the length of maximum and rotation mouth opening and masseter thickness according to the presence or absence of TMJ pain. It was found that there was a significant difference in mouth opening between the TMJ group and the control group in this study. The rotation movement of the TMJ takes place until the incisors are 2.0–2.5 cm apart, and then a sliding or translation movement is performed.3 Giro et al. (2016) suggested that damage to the mandibular muscle and joint impairment may limit the range of motion.21 In addition, changes in the TMJ and neuromuscular control affect pain, which alters the direction and precision of TMJ movement.
In this study, the TMJ group subjects opened their mouths an average of 3.4 cm, demonstrating a limited opening compared to the normal opening of 5 cm. However, this value was within the functional opening range (3.75 cm). Therefore, the subjects in the TMJ group used their TMJs functionally, and they could be considered as experiencing mild TMJ disorders rather than severe difficulties in their daily lives.
There was no significant difference in the asymmetry of the masseter thickness. We thought that a patient with mild TMJ pain did not show any asymmetry of the masseter thickness, and pain or weakening of the masseter. In previous studies, patients with TMJ pain had an increased thickness of the masseter muscle. Ariji et al. (2004) reported that patients with TMJ pain exhibited a thickening of the masseter muscle that was associated with muscle edema.22 However, similar to this study, others have reported that there is no statistically significant difference in the thickness of the muscles according to the presence or absence of TMJ pain.23 Therefore, although masseter asymmetry is not closely related to TMJ pain, it is thought that the decrease in rotation mouth opening is closely related.
The limitations of this study are as follows. This study recruited subjects with and without TMJ pain. With the average mouth opening range of the TMJ group being 3.4 cm, this group does not represent patients with TMJ disorders with severe pain. Therefore, it is difficult to generalize the results of this study to all patients with TMJ pain. Also, since this study was a cross-sectional experiment, we could not observe subjects in the long term. Therefore, in future studies, more subjects and patients with a range of TMJ pain levels should be studied prospectively.
CONCLUSION
The purpose of this study was to compare the length of mouth opening and asymmetry of masseter thickness between the TMJ and healthy group. It was found that there was a significant difference in the amount of rotation and translation opening between the groups. Therefore, exercise programs for patients with TMJ pain should include efforts to increase the amount of rotation and translation opening without TMJ pain. In contrast, there was no significant difference in the asymmetry of the masseter thickness.







