INTRODUCTION
During hip flexion, it is important to distinguish femoral motion from pelvic motion.1–2 Because hip joint and pelvis move sequentially during hip flexion, clinicians commonly attempt to detect the onset of pelvic rotation when measuring the range of hip flexion, or to limit pelvic movement when measuring hamstring muscle length.1,3 However, previous studies have demonstrated concurrent movement of the femur and pelvis, posterior tilting of the pelvis, and flattening of the lumbar spine during hip flexion; collectively, these movements are termed pelvifemoral rhythm.4–10 The contribution of pelvic rotation to hip flexion onsets at a very early point and then persists throughout the range of hip flexion.4–10 Thus, clinicians must consider simultaneous pelvifemoral rhythm when measuring the range of hip flexion or hamstring muscle length.
In previous studies, pelvic motion accompanying hip flexion was analyzed using various tools, including tape lines4–6 or tape markers,9 spherical reflective markers,7, 8, 10 and magnetic sensors.11 However, these tools require time and effort for installation and analysis of the acquired data, and are not easy to apply in clinical settings. Although observation and palpation of the pelvis have been commonly used to measure the range of hip flexion or hamstring muscle length, its sensitivity is insufficient for the detection of early onset movement and cannot quantitatively measure pelvic rotation. The pressure biofeedback unit (PBU) is already commonly used in clinical settings to detect and retrain pelvic movement patterns during lower limb movements,12–14 and should therefore be investigated as an alternative tool to measure pelvic movement during hip flexion.
Tightness of the posterior hip muscles or joint capsule can cause excessive substitutive pelvic motion in the sagittal plane during hip flexion.15 Specifically, because the proximal attachment of hamstrings occurs at the ischial tuberosity, hamstring tension influences pelvic movement during hip flexion.7 Previous studies have reported that the contribution of posterior pelvic tilting to hip flexion is greater in individuals with shorter hamstrings, and in knee extension rather than flexion.7,8 However, no study has yet investigated changes in pelvifemoral rhythm during hip flexion following hamstring stretching. If pelvic movement can be measured indirectly by a PBU during hip flexion, then the relationship between changes in biofeedback pressure recorded by the PBU and the pelvic angle accompanying hip flexion after hamstring stretching could be examined.
Numerous studies have examined pelvic rotation following hip flexion in various postures, including supine,4–7, 9 standing upright,10 and hanging by the hands from a bar.8 Hip flexion maneuvers have been compared between passive and active motion, between unilateral and bilateral motion, and between knee extension and flexion.4–10 In the current study, we examined hip flexion during passive straight leg raising (PSLR) because PSLR is commonly used as a clinical test of hamstring muscle length. Therefore, the objectives of this study were to 1) determine the relationship between pelvic motion and biofeedback pressure measured by a PBU during PSLR and 2) identify changes in biofeedback pressure during PSLR immediately following stretching in subjects with short hamstrings. We hypothesized 1) a positive relationship between pelvic rotation and biofeedback pressure and 2) decreased biofeedback pressure during PSLR after hamstring stretching in subjects with short hamstring.
METHODS
Twenty young adults (14 men and 6 women; mean age, 23.95±1.96 years; mean body height, 168.25±7.69 cm; mean body mass, 66.6±10.46 kg) with short hamstring muscles participated in this study. The sole inclusion criterion was >20° bilateral knee extension, as measured by the active knee extension (AKE) test.16 The following exclusion criteria were applied: (1) lower back pain, (2) history of lower limb pain or previous hamstring injury, and (3) participation in sports or any specific exercise program requiring lengthening of the hamstring within 3 months prior to the study. The sample size was calculated using G*Power software. We used a two-tailed t-test for dependent samples (α = 0.05, effect size = 0.7) to determine that a sample size of 20 was required to achieve 90% power. This study was approved by the Institutional Review Board (IRB) of Joongbu University. All participants were verbally informed of the experimental procedure, objectives, and risks of the study, and provided written informed consent prior to participation.
A digital goniometer (Dualer IQ; J Tech Medical Industries, Heber City, UT, USA) was used to perform the AKE test, and during PSLR in 10° increments. We used a CMS20 ultrasound-based motion analysis system (Winspine for triple lumbar; Zebris Medizintechnik GmbH, Isny, Germany) to measure the pelvic angle in real time during PSLR. This three-dimensional (3D) motion equipment consists of two triple ultrasound transmitters with belt attachments and a fixed system of three microphones. The pelvic angle was calculated by using the microphones to determine the spatial coordinates of the ultrasound transmitters, at a sampling rate of 50 Hz, using the Winspine 2.22 software. This system has been validated in several spinal motion studies.17–19 A PBU (Stabilizer Pressure Biofeedback Unit, Chattanooga Group Inc., Hixson, TN, USA) was used to determine changes in pressure in the lumbopelvic region during PSLR before and after hamstring stretching.
All measurements were conducted with participants in a supine position on a wooden table. Only the right leg was tested. Before and after hamstring stretching, the AKE test was performed to determine changes in hamstring length.19 Subjects were placed in the supine position, with the hip and knee flexed at 90° and the anterior thigh touching a cross-bar to maintain hip flexion. A digital inclinometer was attached below the fibular head using an elastic strap. The starting position was calibrated to 0° at 90° knee flexion in the horizontal position. Subjects were then asked to actively extend the leg until the point of limitation, keeping the feet relaxed without ankle dorsiflexion and the thigh against the bar. The AKE angle (degree of knee extension relative to initial knee flexion) was recorded again in the final position. The AKE angle was defined as the degree of knee flexion from complete knee extension. AKE angles were recorded in triplicate before and after hamstring stretching.
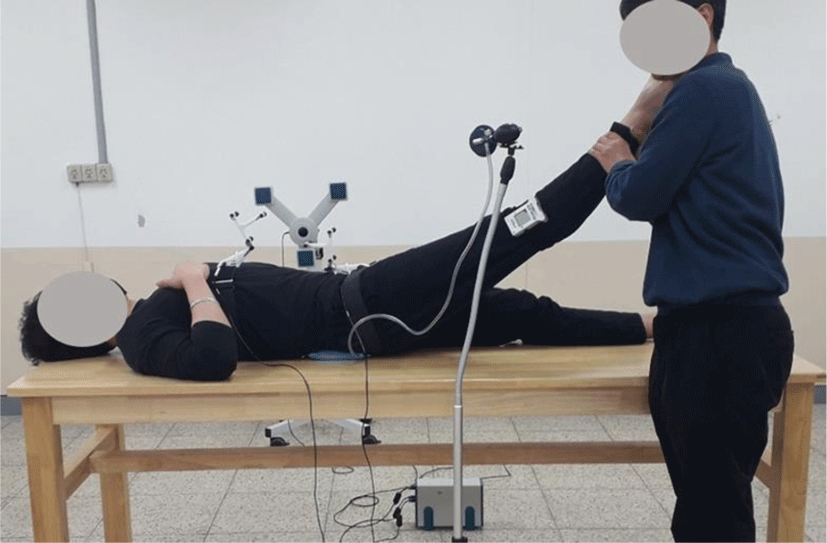
The experimental setting showed in Figure 1. To measure pelvic angle and biofeedback pressure during PSLR before and after hamstring stretching, we mounted the motion analyzer microphones at a distance of 80 cm from the measured leg. A digital goniometer was attached with a strap halfway along the femur shaft to conduct measurements during PSLR at 10° increments until hip joint flexion reached 70° (Figure 1).20 To measure the pelvic angle, one belt holding a triple ultrasound transmitter was attached firmly at the thoracolumbar junction to isolate pelvic movement, and another was attached at the level of the anterior superior iliac and posterior superior iliac spines.16 A PBU airbag was placed under the lumbar spine (L1–S1), centered at the L3 spinous process above L4, and was palpated between the tops of the left and right iliac crests. The airbag was inflated to a base pressure of 40 mmHg and the pelvic angle was calibrated to 0° in the supine position. The experimenter then raised the straight leg in 10° increments during PSLR, from 0° to 70°, at a movement velocity of approximately 5° s−1. Each position was held for 5 s, while biofeedback pressure and pelvic angle were recorded. Subjects feeling pain during PSLR were not asked to raise the leg further.20 To determine the test–retest reliability of PBU measurements, we followed the same procedure with 10 subjects, 2 weeks prior to the study.
Hamstring stretching was performed twice; AKE stretching was always performed before PSLR stretching. Stretching lasted approximately 3 minutes. This static stretching was repeated three times with 10-s rest periods between each stretch; stretching positions were held for 15 s. Hamstring stretching was performed and monitored by the primary experimenter. The subject was asked to relax the lower extremity during stretching, and verbal feedback was provided throughout the stretching protocol to ensure that the lumbar spine and pelvis were maintained in a neutral position.
To perform AKE stretching, each subject was asked to actively and gradually extend the lower leg in the AKE test position until as much stretching force as possible was applied without pain. Once this position was achieved, the subject held it for 15 s. PSLR stretching was performed with the experimenter standing beside the dominant leg, slowly raising the leg perpendicular to the planar surface with one hand placed under the ankle joint and the other hand placed above the knee joint. The subject was asked to inform the primary experimenter when strong but tolerable discomfort was felt during the stretch. The lower extremity was then lowered by a few degrees from this symptomatic position.
The test–retest reliability of PBU measurements was assessed using interclass correlation coefficients (ICC3,1) (95% confidence interval [CI]) and standard error of measurement (SEM). Degree of reliability bases on ICCs was defined as following: <0.70=poor, 0.70–0.79=moderate, 0.80–.89=good, and 0.90–0.99=excellent. Pearson product moment correlations were used to describe the relationships among PSLR angle, biofeedback pressure, and pelvic angle. Simple linear regression analysis was performed to predict biofeedback pressure according to the pelvic angle. Paired t-tests were used to determine significant differences in AKE angle, biofeedback pressure, and pelvic angle, using the PSLR angle before and after hamstring stretching. Statistical significance was determined at a level of p<0.05. Data were analyzed using SPSS software (ver. 10.0; SPSS Inc., Chicago, IL, USA).
RESULTS
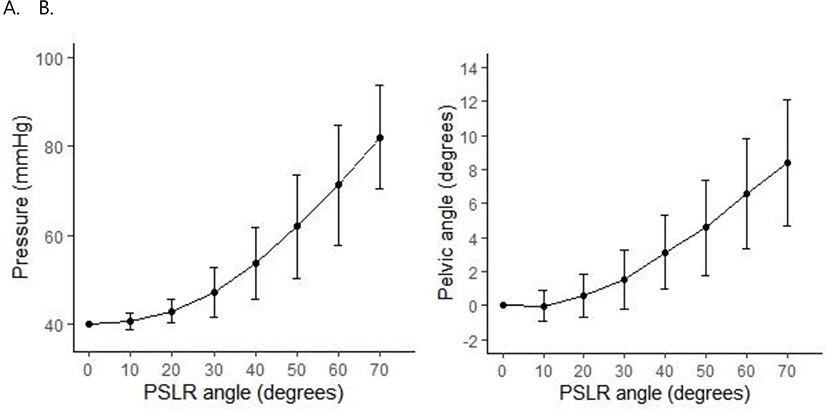
Test–retest reliability analysis showed excellent reliability for PBU measurements (ICC3,1=0.94–0.99; SEM=0.47–0.84 mmHg). There was a significant relationship between pelvic angle and PSLR angle (Pearson’s r=0.75, p<0.05), between biofeedback pressure and PSLR angle (Pearson’s r=0.80, p<0.05), and between pelvic angle and biofeedback pressure (Pearson’s r=0.76, p<0.05) (Figure 2 and 3). The linear regression equation for pelvic angle as an independent factor (R2=0.57, p<0.05) was as follows:
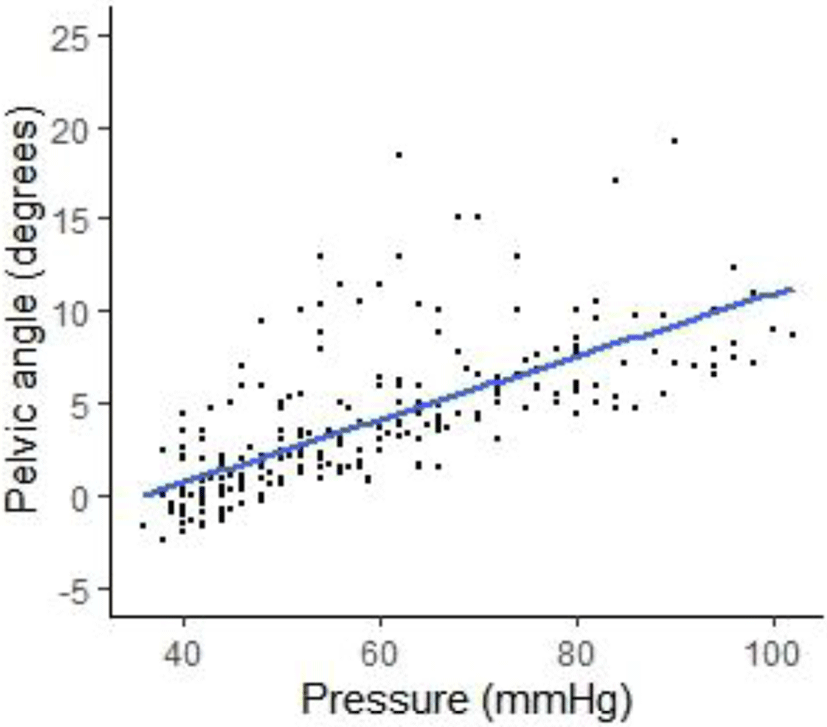
The AKE angle was significantly less post-stretch (mean ± standard deviation [SD]=27.77°±6.16°) than pre-stretch (mean±SD=36.85°±6.68°) (p<0.01). Biofeedback pressure decreased significantly within a PSLR range of 10–60°, and pelvic angle decreased significantly at PSLR angles of 50° and 60° after hamstring stretching (p<0.05) (Table 1).
DISCUSSION
The present study obtained clinically acceptable reliability values for PBU pressure measurements during PSLR (ICC3,1=0.94–0.99). There was a significant linear relationship between biofeedback pressure and pelvic angle. These findings indicate that biofeedback pressure can be measured reliably as result of pelvic movement during PSLR. Azevedo et al.12 reported intra-rater reliability values for biofeedback pressure during AKE of 0.75, 0.77, and 0.79 at 30°, 60°, and 90° knee flexion, respectively. The higher reliability values found in the current study can be explained by the type of lower limb movement examined; the previous study measured biofeedback pressure during active movement to assess lumbopelvic stability, whereas the current study measured biofeedback pressure during passive movement to test hamstring muscle length. Biofeedback pressure measurements may be more reliable during PSLR than during AKE testing because the lumbopelvic movements change with subject’s effort during AKE testing.
The significant linear relationship obtained between pelvic and PSLR angles in this study was consistent with the results of previous studies describing pelvifemoral rhythm. Previous studies have reported that the mean contribution of the pelvic angle to total hip flexion ranged from 8.0% to 37.5%. PSLR was performed as a hip flexion task in two such studies, which reported that the pelvic angle contributed 22.9° (26.8%) to a total PSLR angle of 85.5° 4 and 32.1° (36.9%) to a total PSLR angle of 87.3°.5 Our pelvifemoral rhythm results showed that pelvic motion contributed 8.39° (11.99%) to a total PSLR angle of 70°, which was calculated using mean values obtained before and after hamstring stretching. We infer that the contribution of pelvic movement to total PSLR excursion in the current study was less than that reported in previous studies for two reasons. First, due to differences in total PSLR excursion, pelvic angles reported in previous studies were greater than that determined in this study. Second, previous studies did not isolate pelvic movement from movement of the lower thoracic region, whereas we measured pelvic movement selectively, by attaching triple markers to the thoracolumbar junction.
The hypothesis of this study was that biofeedback pressure would increase with posterior tilting of the pelvis and flattening of the lumbar spine in the sagittal plane during PSLR. We detected a positive linear relationship between pelvic angle and biofeedback pressure in subjects with short hamstring. As similar to this study, a previous study a positive linear relationship between pelvic angle and biofeedback pressure in subjects with normal hamstring.20 PSLR is a clinical test commonly used to measure hamstring muscle length. Our findings indicate that biofeedback pressure measured by a PBU can be employed to measure pelvic movement during hamstring muscle length assessments, for example when the cross-sectional area of the muscle is used as an indicator of muscle strength. According to our regression equation, an increase in pelvic movement by 1° would lead to an increase in biofeedback pressure of 3.35 mmHg. For example, a 5° increase in pelvic angle produces a biofeedback pressure estimate of 62 mmHg.
Previous studies have reported that the contribution of pelvic tilting to hip flexion begins very early and is continuous throughout the range of hip flexion, similar to the contribution of scapular upward rotation to shoulder elevation.5–8, 10, 11 In the current study, both biofeedback pressure and pelvic angle began to increase after 10° of PSLR in most subjects. As previously reported,21–23 the results of the current study suggest that measuring the range of hip flexion as the thigh angle relative to the horizontal plane at the point of perceived onset of the lumbopelvic movement is inappropriate. Thus, clinicians need to be aware of the concurrent pelvifemoral rhythm when measuring the range of hip flexion.
Hamstring flexibility has been proposed as a predisposing factor for non-specific low back pain. 24 Tight hamstrings can restrict hip motion, thereby increasing lumbopelvic motion and causing back pain due to its influence on lumbopelvic rhythm during forward bending.25 Although several studies have reported the immediate effects of hamstring stretching on range of motion, and a reduction in tension and stiffness in the muscle–tendon unit,26–28 no studies have determined the effect of hamstring stretching on pelvifemoral rhythm during PSLR. Our results show that pelvic motion contributed 9.39° (13.41%) and 7.39° (10.56%) to a total PSLR angle of 70° before and after hamstring stretching, respectively. These findings demonstrate that hamstring stretching immediately before and after PSLR changed the pelvifemoral rhythm by decreasing pelvic motion during PSLR.
This change in pelvifemoral rhythm was associated with a decrease in biofeedback pressure during PSLR after hamstring stretching. Improved hamstring flexibility decreased the posterior tilting of the pelvis and lumbar spine flexion. The PBU airbag under the lumbopelvic region received less pressure during PSLR after stretching than before. Therefore, change in hamstring length can be indirectly detected based on pelvic angle and biofeedback pressure, as measured by a PBU during PSLR. Biofeedback pressure decreased significantly at a PSLR angle range of 10–60°; however, pelvic angle decreased significantly only at PSLR angles of 50° and 60° after hamstring stretching. This result indicates that biofeedback pressure is more sensitive than pelvic angle to changes in PSLR angle after hamstring stretching.
There were some limitations to this study. First, we did not exclude other factors affecting the pelvifemoral rhythm during PSLR. In addition to hamstring flexibility, pelvic motion and biofeedback pressure can be influenced by stiffness in single-joint muscles (e.g., gluteus maximus) and the posterior capsule and ligament around the hip joint. Second, biofeedback pressure values were recorded from the PBU without normalization. To compare PBU measurements between individuals, a normalization procedure is required. Future studies must develop normalization protocols for PBU measurements obtained during PSLR. Finally, the results of our study cannot be generalized because only young subjects with short hamstrings participated without control group. Therefore, it is needed to compare the difference of biofeedback pressure and pelvic angle during should be investigated between subjects with and without hamstring stretching in future study.
CONCLUSION
We detected a positive linear relationship between biofeedback pressure measured by a PBU and pelvic angle during PSLR in subjects with short hamstrings. Immediate hamstring stretching tended to decrease pelvic angle and biofeedback pressure during PSLR. Therefore, we recommend the use of a PBU to indirectly measure the degree of pelvic motion when testing hamstring length after stretching.







