INTRODUCTION
Normal muscle activity of the serratus anterior (SA) is essential in the alignment of the scapula and its function of motion.1,2 SA muscle weakness leads to changes in the movement of the scapula, resulting in shoulder pain3,4 and delayed movement,5 being one of the causes of scapular dyskinesis.6 Therefore, scapular protraction exercises have been suggested for weakness of SA,5-7 as a way to strengthen it. Previous studies have mentioned that scapular protraction exercises are effective in increasing SA muscle activity.1,4 In particular, push-up plus exercise along with scapular protraction exercise was found to be more effective than the conventional push-up because it increases SA activity while minimizing the activity of the upper trapezius (UT).3,7 Previous studies suggested that 120° forward flexion is combined with scapula protraction, scapular upward rotation and posterior tipping contributing to increased SA muscle activity.4
Moseley et al.8 stated that 95% of the maximum muscle strength of SA occurs when the angle of shoulder flexion is between 120° and 150°. Exercises including forward flexion, push-up plus, and wall slide that are effective in strengthening the SA muscle have been suggested in many studies. In particular, although push-up plus effectively increases SA muscle activity, it was found that wall slide exercise is more effective than push-up plus since the exercise is performed at a flexion of ≥90°.9 In addition, SA muscle activity increased more when push-up plus was performed at 120° of shoulder flexion than during general push-up plus exercise.10 Therefore, it can be observed that exercising with a shoulder flexion of ≥90° is more effective in enhancing SA muscle activity.
Another study on SA activity has suggested exercising by touching an unstable surface at an end position of scapular protraction.1,3,7 It was found that exercising by touching an unstable surface during scapular protraction helps for shoulder rehabilitation as well as recovery of muscle activity.3 In addition, using an unstable surface in scapular protraction increases SA activity to a higher level than that performed at stable status.1,3,8 In contrast, Lehman et al.11 reported no major difference between scapular protraction exercises on stable or unstable surfaces in SA muscle activity. Because a contact surface are inconsistent and controversial during push-up plus as a closed kinetic chain exercise. The resistance of scapular protraction during push-up plus is proportionate to the weight. Since using weight as resistance in push-up plus may cause excessive resistance on scapular protraction, high co-activation of muscles surrounding the shoulder joint was occurred during scapular protraction exercise.7,10
Therefore, adjustable resistance is essential to decide the effectiveness of scapular protraction exercises for the selective activation of SA. Jung et al.12 invented a method of controlled resistance itself by suggesting the scapular protraction exercise with self-resistance at 120° of shoulder flexion. However, there has been no study comparing SA muscle activities in performing forward flexion with protraction (FFP), FFP with self-resistance (FFPS), FFPS with a hand-exerciser (FFPSH) at 120° of shoulder flexion.
The purpose of this study is to investigate the effect on SA muscle activity while performing self-resisted scapular protraction exercise at 120° of shoulder flexion using unstable surfaces in a sitting position. The hypothesis was that FFPSH exercise would show a statistically significant increase in SA muscle activity compared to FFP and FFPS exercises.
METHODS
Twenty healthy individuals were participated (age=22.8±5.3 years; height=167.7±9.6 cm; weight=64.3±6.5 kg). Inclusion criteria were (1) no pain while performing scapular protraction exercise at 120° of shoulder flexion and (2) no diseases of the nervous and musculoskeletal systems. Exclusion criteria were (1) medical history of shoulder or elbow surgery and (2) pain in shoulder or elbow joints. The protocol of experiment was explained in detail to all participants, and prior written consent was obtained from each participant. This study was approved by the Institutional Review Board of Hoseo University (1041231-210615-HR-127-01).
A measurement program was used for analyzing muscle activities of SA, UT, and pectoralis major (PM). An electromyography (EMG) (TeleMyo 2400T, Noraxon, USA) device was used. The band pass filter was set at 20–450 Hz, and the sampling rate at 1024 Hz. The signal for all the muscle activities was processed by using a root mean square value of 50 ms (moving window). Before placing the electrodes, the area where electrodes are to be attached was shaved. Then, the skin was cleaned with an alcohol swab. Ag/AgCl surface electrodes were applied to the relevant area. Two separated bipolar surface electrodes were placed 2 cm apart. An electrode was attached to the middle part of muscle belly as the guideline of Rainoldi et al.13 EMG patches were applied by following the guideline of Cram et al.14 to measure SA, UT, and PM muscle activities. The EMG signal was acquired using MyoResearch® XP Master Edition software. Muscle tests for the maximum voluntary isometric contraction (MVIC) of SA, UT, and PM were performed according to the guideline of Kendall et al.15 Muscle contraction was standardized using %MVIC. The signal of muscle activities was recorded while each participant was maintaining scapular protraction of their dominant side for 5 seconds at the target bar. The signals at 2– 4 seconds were analyzed, excluding each 1 second at the beginning and end of exercise.16
Participants performed three different scapular protraction exercises using their dominant arms. Subsequently, each exercise was performed three times for 5 seconds each, with 5-minute rest between exercises. The order of the three different exercises was in random order. The exercises were standardized by using a metronome set at 60 bit/minute.
Each participant sat on a chair with backrest as an initial position. The dominant shoulder was flexed to 120° with the trunk straight in a sitting position on the chair on even ground (Figure 1). While the shoulder of the dominant side was flexed at 120°, scapular protraction was fully performed in a neutral posture with the elbow fully extended. The target bar was set at the position in which each participant can perform scapular protraction without bending and rotating the torso. Each participant maintained scapular protraction for 5 seconds with the dominant hand clenched at the target bar without shoulder elevation and trunk rotation guided by the researcher.
Each participant was instructed to wrap the fist of the dominant side with the hand of the nondominant side while flexing the dominant shoulder at 120° at the initial position (Figure 2). Self-resistance was provided while the fist of the dominant side was pushing against the nondominant hand, which was pulling the fist of the dominant hand simultaneously. Both elbows were fully extended, and scapular protraction was fully performed for 5 seconds without shoulder elevation and trunk rotation guided by the researcher.
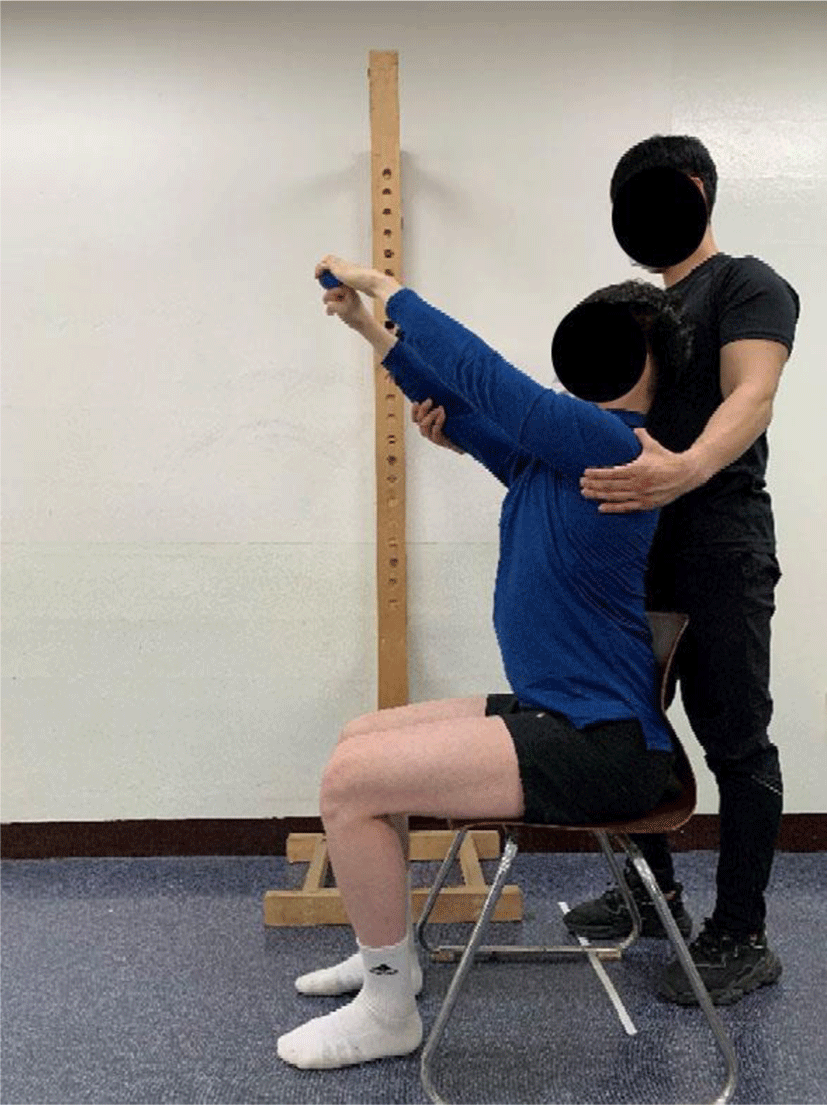
Protraction of the dominant scapula was performed similar to FFPS, while providing self-resistance to the nondominant hand gripping a hand-exerciser (Thera-Band Hand Exerciser; The Hygenic Corporation, Akron, OH), a rubber ball. Hand-exercisers are in different colors to show the approximate resistance occurring during compression of approximately 50%: yellow represents a resistance of 0.68 kg, green 1.36 kg, and blue 3.64 kg. 17 The hand-exercisers used in this study were all blue. The hand-exerciser was placed between the fist of the dominant side and the nondominant hand, and the elbow was fully extended when the shoulder of the dominant side was flexed at 120° while providing self-resistance to the hand with a hand-exerciser and scapular protraction fully performed for 5 seconds without shoulder elevation and trunk rotation guided by the researcher (Figure 3).
To determine that all the variables were normally distributed, Kolmogorov–Smirnov test was used. Repeated measurement of one-way analysis of variance was used to compare muscle activities and proportions of SA, UT, and PM muscles during scapular protraction exercise. All the data of this study were analyzed by using IBM SPSS statistics 20.0 (SPSS Inc, Chicago, IL). In case significant interactions was confirmed among exercises, the Bonferroni correction was set at 0.017 (0.05/3) at a statistically significant level.
RESULT
A statistically significant difference was identified in the muscle activity of SA and SA/UT ratio during three different scapular protraction exercises (p<0.01) (Table 1). The statistically significant difference of SA muscle activity during FFPSH was higher compared to that during FFP and FFPS (Table 1). In addition, a statistically significant increase in SA/UT ratio was identified during FFPSH compared to that during FFP and FFPS exercises (Table 2). However, no significant difference was identified in terms of UT, PM muscle, and SA/PM muscle ratio (p>0.05; Tables 1 and 2).
FFP, Forward flexion with protraction; FFPS, Forward flexion with protraction with self-resistance; FFPSH, Forward flexion with protraction with self-resistance with hand-exerciser; SA (dominant), serratus anterior; UT (dominant), upper trapezius; PM (dominant), pectoralis major; SD, Standard deviation.
| Ratio | Positions | F value | p value | ||
|---|---|---|---|---|---|
| FFP | FFPS | FFPSH | |||
| SA/UT | 1.66 | 3.54* | 4.40* | 7.68 | <0.01 * |
| SA/PM | 2.45 | 3.39 | 3.59 | 3.59 | 0.074 |
FFP, Forward flexion with protraction; FFPS, Forward flexion with protraction with self-resistance; FFPSH, Forward flexion with protraction with self-resistance with hand-exerciser; SA (dominant), serratus anterior; UT (dominant), upper trapezius; PM (dominant), pectoralis major; SD, Standard deviation.
DISCUSSION
Scapular protraction exercise of shoulder flexion at 120° has been applied in strengthening SA.3,7,10 This study aimed to compare muscle activities of SA, UT and PM while performing three different types of scapular protraction exercises among FFP, FFPS, and FFPSH.
From the results of this study, a significant increase was identified in terms of muscle activity of SA and SA/UT ratio in FFPSH exercise than that in FFP and FFPS exercises. Therefore, we identified that providing self-resistance to an unstable surface by using a hand-exerciser in the dominant hand while performing scapular protraction at 120° of shoulder flexion during FFPSH was more effective in increasing SA muscle activity than FFP and FFPS exercises.
There were some reasons for the difference in FFPSH exercise compared to FFP and FFPS exercises. First, the reason for increased SA muscle activity in FFPSH compared to that in FFPS exercise was that the hand-exerciser held at the distal extremity provided an unstable surface, and self-resistance was offered using the nondominant hand. Because of those, mechanoreceptors might have been stimulated, and hence, a condition in which more stability is required to the proximal extremity including the scapula.18 This might have contributed to increased SA muscle activity, which directly affects the stability of the proximal extremity. Previous studies reported that push-up plus in a closed kinetic chain posture on an unstable ground surface using Togu or a Swiss ball is not effective in increasing SA muscle activity.1,11 In case of Togu and a Swiss ball, because considerable pressure occurs with the weight during push-up plus posture, it may be possible that the unstable surface is fixed at one point, in accordance with the occurrence of high pressure at the end position of scapular protraction.11 Therefore, the instability of the contact surface may be minimized while Togu or a Swiss ball was compressed in a closed kinetic chain position by weight.11 Therefore, there was major difference between the surface with the weight bearing and the nondominant hand with no weight applied. In this study, while the nondominant hand for self-resistance, was not fixed, providing an unstable contact surface while pressing a hand-exerciser at the end of the fist of the dominant side can contribute to increased SA muscle activity.
Second, the reasons of significant increase in SA/UT ratio during FFPSH than that during FFP and FFPS exercises are as follows: UT activity was minimized because scapular protraction and elevation were controlled using the nondominant hand during FFPSH. In previous studies, SA/UT ratio of the posture in which self-resistance was provided at 120° of shoulder flexion was higher than that during scapular protraction without self-resistance.12 Our findings show decreased UT muscle activity during FFPS and FFPSH exercises with self-resistance and increased SA muscle activity during FFPSH exercise. Therefore, increased SA/UT ratio during FFPSH compared to FFP and FFPS could have occurred because SA muscle activity increased to the maximum when a hand-exerciser was used. In addition, SA muscle activity increased during FFPS and FFPSH than that during FFP. Because the controlled self-resistance for FFPS and FFPSH was provided using the nondominant hand during scapular protraction occurred at 120° of shoulder flexion.12
In general, performing scapular protraction at ≥90° is more effective in increasing SA muscle activity.10,19 Shoulder flexion at 130° showed a higher increase in SA muscle activity than shoulder flexion at 90° in previous studies.20 Wall slide exercise performed at 120° of shoulder flexion as a type of open kinetic chain exercise, is more effective in increasing SA muscle activity compared to push-up plus performed as a type of closed kinetic chain exercise.9 In this study, FFPSH can be selectively applied to the side with SA weakness, and this may be used to minimize possible pain and impingement in the shoulder joint instead of weight-bearing exercise. Therefore, when pain occurs in the glenohumeral joint while performing the push-up plus exercise in a prone position bearing the weight, it is considered that FFPSH can be applied as an alternative. Along with FFPSH exercise, self-resistance through an unstable surface during scapular protraction exercise at 120° of shoulder flexion can be recommended as an effective SA strengthening exercise.
There are several limitations in this study. First, only young and healthy male individuals participated. So it cannot be generalized to different generations and sex as well as to patient groups with shoulder impingement syndrome. Second, muscle activities and onset times of the surrounding muscles of the shoulder joint were not measured. Further studies on the surrounding muscles are required. Third, although the use of surface electromyogram included superficial activities of the muscles, this study lacks research on muscle activity in the deep part of muscles. Fourth, the pressure and the distance given to the hand-exerciser during FFPSH exercise were not measured.









