INTRODUCTION
Stress urinary incontinence (SUI) is defined involuntary loss of urine on exertion, effort, sports activities, coughing or sneezing1,2 and is widespread,3 although it seems to be undertreated.4 Pelvic floor muscle (PFM) training is suggested as first-line and non-invasive intervention for SUI.5 PFM training has discouraged compensatory muscle contractions such as abdominals, gluteals and hip adductors.6,7 Although it is difficult to contract accurately the PFM,6,8 the concern remains that compensating other muscle activity would detract from a proper contraction of the PFM.9
SUI could be related to musculoskeletal dysfunction, such as low back and pelvic pain and sacroiliac joint dysfunction. Poor control of the PFM, including the levator ani, sphincter muscles, and urogenital diaphragm can be contribute to SUI.9,10 Strengthening of PFM has been applied to improve symptom of incontinence in female.7,11 Other muscles of the pelvis and hip have been linked to PFM dysfunction. 12 PFM alone is difficult to maintain sufficient tension or produce enough force to encounter intra-abdominal pressure and maintain continence during jumping and sneezing, where female with SUI often areal difficulty maintaining continence.12 This indicates that other anatomical structures, such as connective tissue, fascia and additional muscles (abdominal and hip muscles) would be important contributors to normal PFM function.12 Because, in particular, the obturator internus shares a fascial attachment with the PFM, the obturator internus could affect PFM function and tension of endopelvic fascia.13
Previous studies have confirmed the relationship between auxiliary muscle contractions and PF muscle activity. Bo and Stien have confirmed PFM activity during gluteal and hip adductor contractions.14 Sapsford et al. have demonstrated a relationship between PFM activity and transversus abdominis contractions.15,16 Underwood et al. have reported significant weakness in the hip abductors of female with SUI when compared with healthy controls.17 However, no studies have investigated the correlation between hip muscles and PFM strength.
Thus, the purpose of present study was to investigate the relationship between hip extensor, abductor, adductor and gluteal squeeze strength and PFM strength and endurance in female with SUI. We hypothesize that the hip abductor and extensor strength may be associated with PFM strength and endurance, because of the inexistence anatomical and mechanical association between hip adductors and PFM. It can represent a better choice among hip extensor, abductor, adductor and gluteal squeeze, in clinical practice and protocol for PFM rehabilitation,18 when looking for strategies to improve proprioception and PFM recruitment, as well as facilitating rehabilitation.
METHODS
The participants were recruited by advertisements that provided the telephone contact to the interested parties. After contact, there were scheduled visits to confirm the inclusion and exclusion criteria in the present study.
Inclusion criteria were 1) SUI diagnosed by a urogynecologist, 2) a leakage episode occurring more than once a week, 3) generally healthy (apart from SUI), 4) body mass index < 30 kg/m2, 5) age between 30 and 60 years, 6) non-smoker and 7) not addicted to alcohol or drugs. Exclusion criteria were 1) pregnancy/ planning to get pregnant, 2) pelvic or abdominal surgery within the last six months and 3) PFM and hip muscle training within the last three months 4) concomitant treatment for SUI during the trial period, 5) neurological or psychiatric disease and 6) urinary tract infection.
A priori using G*power (version 3.1.3; University of Trier, Trier, Germany) was used to calculate sample size for a power of 0.80, an α level of 0.05 and a correlation of 0.5. If there is a significant correlation between hip muscles strength and PFM functions, it is the expected value that a correlation of at least 0.5 (moderate effect) would occur. The sample size was required at least 29 subjects.
A total of 33 participants met the inclusion and exclusion criteria (Table 1). Before the study, all subjects were explained about the all procedures of the study and signed an informed consent form approved by the Institutional Review Board of Yonsei University, Wonju (1041849-201802-BM-005-01).
| Women with stress urinary incontinence (n=33) | |
|---|---|
| Age (yr) | 41.6 ± 8 |
| BMI (kg/m2) | 22.7 ± 3.1 |
| Duration of symptoms (yr) | 12.7 ± 11.3 |
| Number of deliveries | 1.7 ± 0.9 |
| Vaginal deliveries | 1.5 ± 1.9 |
From August 2018 to September 2018, PFM strength and endurance were measured at urogynecology clinic in Seoul, Korea and hip muscles strength were measured at laboratory setting. PFM strength was measured first and then, PFM endurance by urogynecologist. Hip extensor, abductor, adductor and gluteal squeeze strength were measured in random order by orthopedic physical therapist. The order of measurement of hip muscles strength was randomized by www.randomization.com.
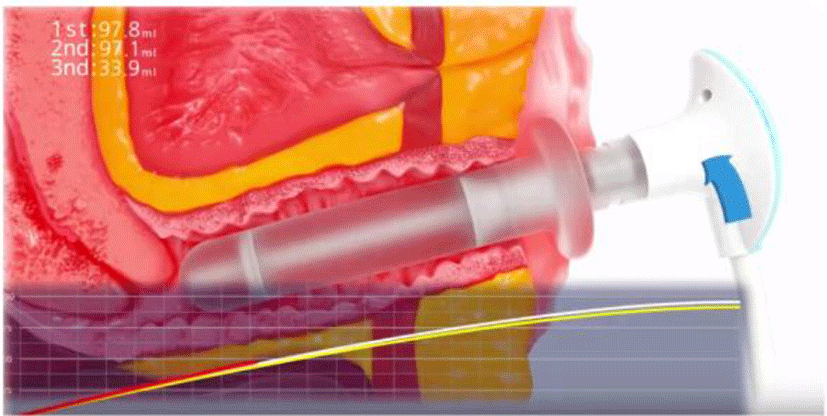
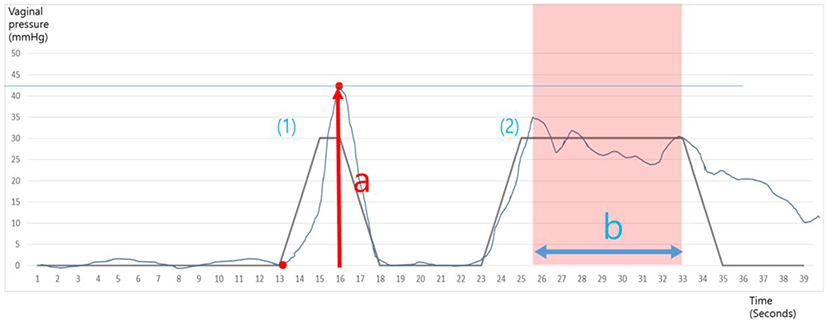
The PFM functions were assessed in hook-lying position by a VVP-3000 perineometer (QLMED Ltd, Gyeonggi-do, Korea) for all participants.19 The vaginal probe in perineometer is 24 mm in diameter and 115 mm in length with inserted vaginal active length of 66 mm and is connected to a microprocessor with latex tubing for transmission of pressure readings when the insert is compressed by vaginal wall (Figure 1). The baseline pressure as mmHg was recorded without voluntary PFM contraction and then was zeroed. We asked for contracting subject’s PFM and to squeeze with maximum voluntary contraction (MVC) perceived effort for three seconds. Participants were instructed to pull their PFM in and up as much as possible without using of abdominal and hip muscles contraction.20 PFM strength was measured from the resting pressure line until the peak, not involving the resting pressure, reported as the mean of two MVC, and recorded as mmHg (Figure 2).21 PFM endurance was measured for the mean of contraction pressure for 10 s, during one attempt and recorded as mmHg (Figure 2).
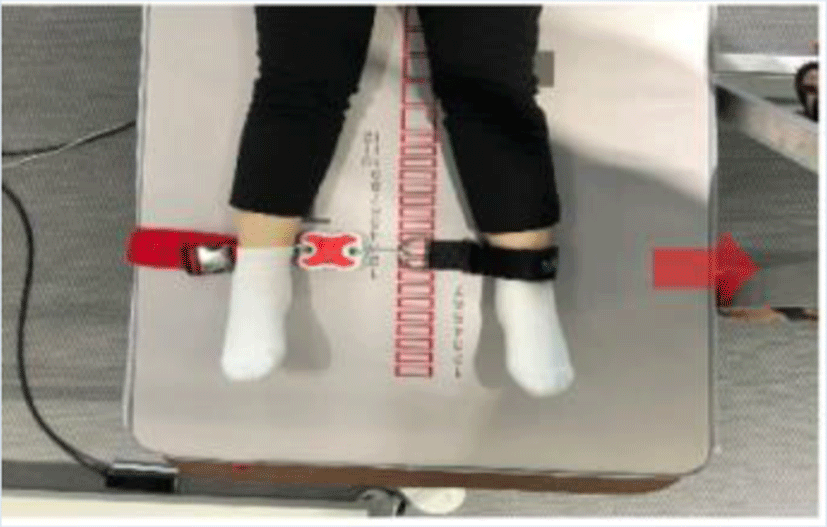
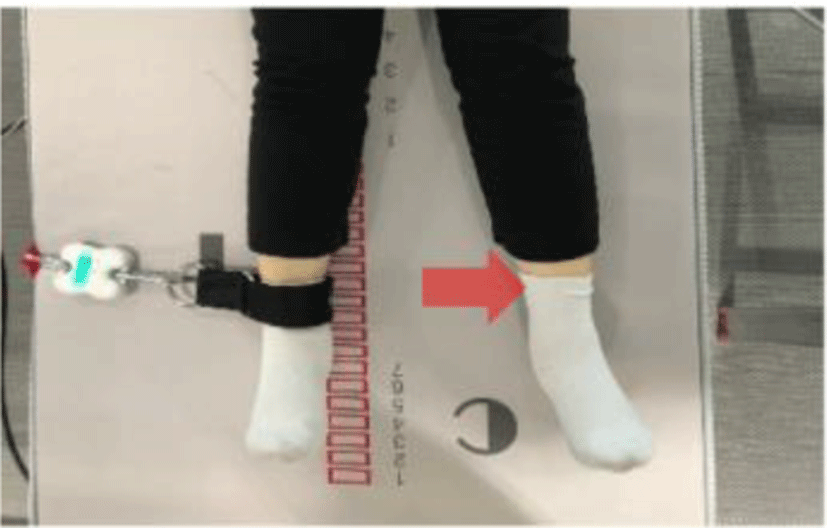
Smart KEMA tension sensor (KOREATECH Co., Ltd., Seoul, Korea) was used to measure isometric strength and to control initial tension on belt by 3 kgf. Tension sensor was measurable up to 1960 N, with an accuracy of 4.9 N and a 10 Hz sampling frequency. The force signals were measured from maximal voluntary isometric contraction of the hip extensor, abductor, adductor and gluteal squeeze strength. Data measured by sensors were transferred to a tablet via Bluetooth device connection and analyzed with the Smart KEMA application (KOREATECH Co., Ltd., Seoul, Korea). Hip muscles strength testing by measured Smart KEMA tension sensor showed excellent intra-(ICC3,1>0.95) and inter-rater (ICC2,1>0.95) test reliability.22
For measurement of hip muscles strength, the belt length was adjusted for measure isometric strength in start position. Participants were asked hold maximal strength for 5 seconds and middle 3 seconds was calculated for average. The hip extensor, abductor and adductor strength were calculated the average value of both side. Table 2 shows the position and procedure for each muscle strength test.
STATISTICAL ANALYSIS
All statistical analyses were performed using SPSS software (ver. 18.0; SPSS Inc., Chicago, IL, USA) with alpha set at 0.05. The Kolmogorov–Smirnov Z-test was applied to confirm the normality of the data distribution. Pearson’s correlation coefficients were constructed to examine the relationships between hip extensor, abductor, adductor and gluteal squeeze strength and PFM strength and endurance. For the r value, an r≥0 and <0.1 was classified as no effect, r≥0.1 and <0.3 was a small effect, r≥0.3 and <0.5 was a moderate effect, and r≥0.5 was a large effect.
RESULTS
Table 3 shows the correlation coefficients between PFM functions and hip muscles strength. There were not significant correlations between PFM strength and hip extensor strength (r=0.078), hip abductor strength (r=0.091), hip adductor strength (r=0.119) and gluteal squeeze strength (r=–0.036) (Table 3). Also, there were not significant correlations between PFM endurance and hip extensor strength (r=0.067), hip abductor strength (r=–0.016), hip adductor strength (r=0.112) and gluteal squeeze strength (r=0.112) (Table 3).
DISCUSSION
The effect of PFM training for SUI have been supported by studies suggesting that PFM training produces greater outcomes than no treatment, inactive control treatment, or placebo drug.11 Our main results do not support our hypothesis, which presents that there were not significant correlations between PFM functions and strength of hip extensor, abductor, adductor, and gluteal squeeze in female with SUI. This hypothesis was based on anatomical supposition that the obturator internus could play role of myofascial force transmission, which is deep hip external rotator muscles and to be connected with the levator ani. Rotator cuff, such as the gluteus maximus and gluteus medius tendons, associated with the hip joint and pelvis.13 However, not only hip adductor strength but also hip extensor, abductor and gluteal squeeze strength were not related to PFM functions.
Strengthening the hip muscles has been recommended as one component of intervention for improving SUI.23 Also, previous studies have suggested that hip abductor, adductor, extensor and external rotator muscles co-contract with PFM contraction.14,24 However, other study only hip abduction strength among strength of hip flexor, extensor abductor, adductor, external rotator and internal rotator differed between female with and without SUI.17 Also, the absolute difference in hip abduction isometric strength between groups was only 2.6% body weight.17 In addtion, the co-contraction of the PFM and the hip adductors or abductors did not increase PFM efficiency about increasing or holding PFM strength.25 Similarly, during a PFM contraction, co-contractions of other muscle (diaphragm, abdominal muscles, hip extensor, hip abductor, adductor, external rotator, and internal rotator) groups did not exceed the intravaginal pressure rise.21
Given the absence or a statistically significant relationship between PFM functions and hip extensor, abductor, adductor and gluteal squeeze strength in this study, one might logically question the rationale for including hip extensor, abductor, adductor and gluteal squeeze strengthening as part of a SUI rehabilitation and intervention strategy. In the present study, the hip external rotator strength was not measured. If obturator internus function is critical to PFM function, the hip external rotator strength may have been selectively correlated with the PFM functions. However, obturator internus only contributes a small proportion to the force generation of the hip external rotators collectively, similarly other muscles (hip extensor, abductor and adductor strength), then hip external rotation strength may be expected to have a poor relationship with PFM functions. Also, the reason for this study result could be the difficulty of co-contraction of hip abductor, adductor, extensor and external rotator muscles with PFM in female with SUI, which is caused by PFM dysfunction. Previous studies have determined the co-contraction of hip abductor, adductor, extensor and external rotator muscles with PFM only in healthy female.14,24 If the ability of PFM contraction is insufficient and dysfunction, it may be difficult to cause co-contraction of the hip muscles and PFM. Therefore, strengthening the hip muscles to stimulate co-contraction of the PFM as a rehabilitation strategy for improving PFM functions, as SUI intervention, may not be an appropriate strategy.
The present study had some limitations. First, the sample size is small. Thus, further study is needed to generalize the experimental results. Second, we did not measure electromyography of hip muscles and PFM for exactly detecting co-contraction. Further study needs to determine activity of hip muscles and PFM during PFM or hip muscles contraction in female with SUI. Third, we did not determine a correlation between hip muscles strength and SUI symptoms or urinary leakage. Thus, further study needs to confirm relationship between hip muscles strength and SUI symptoms or urinary leakage to find the possibility of SUI intervention.
CONCLUSIONS
There were no significant correlations between PFM functions and strength of hip extensor, abductor, adductor, and gluteal squeeze in female with SUI. These findings could indicate the difficulty of co-contraction of hip abductor, adductor, extensor and gluteal squeeze with PFM in female with SUI, which is caused by PFM dysfunction. Therefore, strengthening the hip muscles to co-contract PFM may be difficult to recommend for improving PFM functions in female with SUI.