INTRODUCTION
The European guidelines recommend supervised exercise therapy as a first-line treatment in the management of non-specific chronic low back pain (NCLBP).1 Exercise therapy is effective at improving function and decreasing pain in adults with NCLBP.2 In a systemic review, Middelkoop et al. found 37 studies on the topic of exercise therapy.3 Exercise therapy improved post-treatment pain intensity, disability, and long-term function. There is still no consensus as to what kind of exercise should be used.1 In the European guidelines, recommendations are not given on the specific-exercise to be set about populations with NCLBP.2 Hayden et al. reported no evidence to support the effectiveness of specific-exercise over others in patients with NCLBP. The lack of consistent evidence to support exercise interventions may be due to the heterogeneous study populations for comparison.4,5
Over several years, the custom has been to divide people with NCLBP into homogeneous populations of similar characteristics, in an effort to improve patient outcomes. The Agency for Healthy Care Policy and Research (AHCPR) suggested that optimal clinical management for lower-back problems depends on accurate diagnosis.6 There is growing evidence suggesting that patients with lower back pain can be subclassified into meaningful treatment groups. Homogeneous subgroups may result in more efficient treatment strategies and ountcomes7 and may increase the likelihood of responding to specific treatment.8
Movement system impairment (MSI) subgroups consist of five categories based on the testing of muscular stability, alignment, asymmetry, and flexibility of the lumbar spine, pelvis, and hip. The intervention purpose of subgroups is to correct factors predisposing or contributing to movement pattern impairments, alleviating stress on painful tissues, and allowing inflammation to subside. Spinal dysfunction is prevented and relieved through the optimal alignment and movement of the lumbopelvic region by the trunk muscles.9
Previously, there was intervention study for subjects in rotation with flexion syndrome into MSI subgroups.3 Marcie et al. reported on an intervention study for the rotation with extension syndrome group.10 Previous studies provided information about specific exercise via MSI classification, but case report. In Park et al.’s study, they determined the effects of the abdominal drawing-in maneuver on pelvic motions during active prone knee flexion in RE subgroup.11 Noh et al. suggested restricting pelvic rotation by balancing muscle activity during active straight leg raises in women with NCLBP.12
However, fewer studies have investigated specific interventions via MSI classification of patients with NCLBP. Particularly, no study has compared improving pain and functions between specific interventions via MSI classification and general exercises. Therefore, the aim of the present study was to compare the effects specific exercise in the subgroups via MSI classification and general exercises in patients with NCLBP.
METHODS
This study involved 34 patients with NCLBP who visited Hospital, in Pusan, Korea. Inclusion criteria included an onset of LBP of more than 12 weeks, an oswestry disability index (ODI)>20 points, and a visual analogue scale (VAS) score >2 points. Subjects were randomly grouped into a specific exercise group (n=17) by their MSI classification or a general exercise group (n=17). The MSI group was classified into five subgroups by MIS classification system.
Exclusion criteria were a history of spinal surgery in the previous three months, severe kyphosis, scoliosis or spinal stenosis, scheduled for surgery, history of more than one surgical procedure on the spine, cancer, rheumatoid arthritis, ankylosing spondylitis, neurological disease other than nerve root involvement at the spinal level, and inability to stand and walk without the use of walking aids.13 All participants reviewed and signed consent forms before volunteering, and the Institutional Research Review Committee of Inje University gave ethics approval.
We measured before and after the six-week intervention program. To obtain reliable and valid scores of pain, psychosocial problems, disability, and physical function characteristics, we used the visual analog scale (VAS), fear avoidance belief questionnaire (FABQ),14 Oswestry disability index (ODI), patient-specific functional scale (PSFS),15 finger tip-to-floor test (FF),16 sorensen test,17 and functional movement screening test (FMS).18
Pain levels were evaluated using visual analog scale (VAS; 100 mm). A 0 indicated no pain and 100 mm indicated the worst pain level. For the assessment of psychosocial problems, we used the Korean version of the FABQ (in physical activity and work).14 All participants were asked to complete the study questionnaires at the start and the end of the six-week study period. The ODI and PSFS were used to assess the level of disability associated with the NCLBP. The ODI has a percentage of total score ranging from 0 (minimal disability) to 50 (maximum disability), obtained by computing the sum of all responses. Physical functions used the FF, trunk extensor endurance test to evaluate back extensor endurance, and functional movement screening test as an integrated assessment tool .
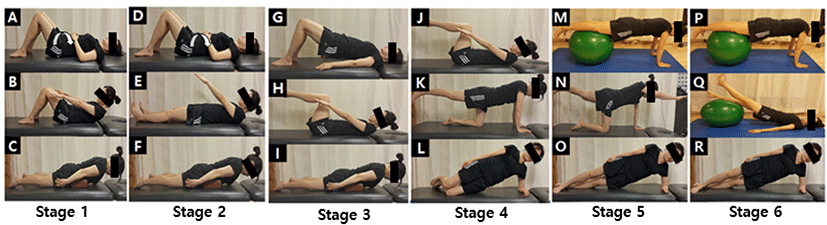
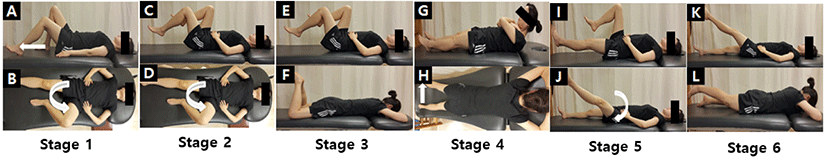
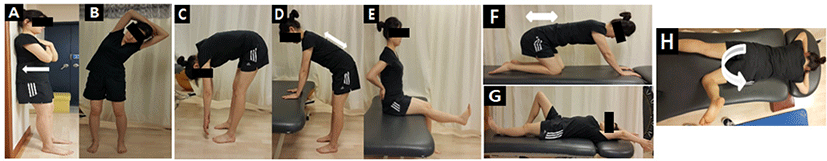
The general and MSI groups performed stretching for 10 to 15 minutes prior to the specified exercises. Both groups visited the hospital exercise center twice a week for six weeks and performed exercises for about 50 minutes. All subjects were instructed in three exercises per stage and holding 10 seconds 10 times for three sets per exercise. The general group applied methods suggested by McGill: pelvic tilting from a lying position, abdominal muscle strengthening exercises, back extensor strengthening exercises, oblique strengthening exercises, and Swiss ball coordination exercises (Figure 1).19,20 The MSI group consisted of strengthening exercises and corrective exercises: abdominal muscles, back extensor, gluteus maximus, and gluteus medius strengthening exercises (Figure 2); standing agains a wall, lateral spinal flexion, forward bending; spinal and hip flexion and forward bending; hip flexion with flat lumbar spine, knee extensions, and dorsiflexion; and rocking backward, latissimus dorsi muscle stretches, and hip rotations (Figure 3).
We measured the mean and standard deviation (SD) of the VAS, FABQ1,2, PSPF, ODI, FF and FMS scores. A two-way analysis of variance (ANOVA) was used to determine the main effect and any interaction between the VAS, FABQ1,2, PSPF, ODI, FF and FMS scores. The within-group factor was time (pre-intervention vs. post-intervention) and the between-group factor was group (MSI vs. general exercise). The significances of differences in demographic between subjects in the MSI and general exercise groups were analyzed by independent t-tests. Statistical Package for the Social Sciences (SPSS) ver. 18.0 (SPSS Inc., Chicago, USA) was used for analyses, and the significance was the adopted value of p<0.05.
RESULTS
The demographic and outcome measures data at baseline did not differ significantly between the two groups (Table 1). A significant time-by-group interaction was observed for the VAS, Sorenson Test, and FMS. An independent sample t-test demonstrated that the MSI exercise group had greater VAS (Table 2; F=8.39, p<0.001, mean difference=21.81 mm), Sorenson test (Table 3; F=8.39, p=0.014, mean difference=34.1 sec.), and FMS (Table 3; F=9.96, p=0.003, mean difference=2.7 point) values. In addition, the post-hoc paired t-test showed that the Sorenson Test (Table 3; p<0.001) and FMS (Table 3; p<0.001) significantly increased post-intervention versus pre-intervention in the MSI exercise group. Also, VAS (Table 2; p<0.001) significantly decreased post-intervention versus pre-intervention in the MSI exercise group.
| Variable (unit) | General group (n=17) | MSI group (n=17) | p |
|---|---|---|---|
| Age (years) | 42.12±13.20 | 45.00±12.93 | 0.525 |
| Body mass index (kg/m2) | 23.42±2.87 | 22.98±2.64 | 0.654 |
| Variable | Group | Pre-intervention | Post-intervention | p | |
|---|---|---|---|---|---|
| Mean±SD | Mean±SD | Within group | Between groups | ||
| VAS (mm) | General | 48.82 ±22.05 | 40.01±20.92 | 0.007* | 0.007* |
| MSI | 49.41±21.64 | 27.65±16.78 | <0.001* | ||
A significant main effect was found for time for pain. VAS significantly decreased in the post-intervention versus pre-intervention in the general exercise group (Table 2; 40.01±2.09 mm vs. 48.82±22.05 mm, p=0.007).
A significant main effect was found for time in the psychosocial problem. FABQ in physical activity significantly decreased in the post-intervention versus pre-intervention in the MSI exercise group (Table 4; 15.53±6.28 vs. 20.76±6.54, p=0.012). FABQ in work significantly decreased in the post-intervention versus pre-intervention in both groups (Table 4; general: 28.24±12.54 vs. 37.35±12.86, p=0.002; MSI: 26.76±13.38 vs. 35.59±11.05, p<0.001). There was no significant difference in psychosocial problems between the groups.
A significant main effect was found for time in disability. PSPF significantly increased in the post-intervention versus pre-intervention in the MSI exercise group (Table 5; 7.76±1.15 vs. 5.58±1.47, p<0.001). ODI significantly decreased in the post-intervention versus pre-intervention in both groups (Table 5; general: 19.29±4.47 vs. 27.18±6.64, p<0.001; MSI: 17.53±7.13 vs. 27.29±7.55, p<0.001). However, there was no significant difference in disability between the groups.
DISCUSSION
We compared the effect of specific exercise by MSI classification and general exercise in patients with NCLBP. Our results show that the MSI exercise and general exercise groups decreased pain, psychosocial problems, and disability, and increased physical function in patients with NCLBP. However, reduced FABQ in physical performance and PSPF were only found in the specific exercise by MSI classification.
In this study, pain significantly decreased in both groups, but the MSI group showed a larger mean difference. Pain could be distributed on unstable segments of lumbar spine in radiological confirmation,16 and could be induced due to muscle imbalance19,21 exaggerating the flexibility of the site.9 Also, pain related to balanced isometric contraction and movement control provided by the trunk muscles.9 The general exercise group performed only strength training of the abdominal and paraspinal muscles.22 Previous studies reported significantly decreased pain in the general exercise-only group after the end of an eight-week exercise period; it is the same with our findings. However, the pain improved in the specific exercise group by MSI classification, likely due to restricted excessive movement of the flexible lumbar segment, as well as strengthening during the exercise.9 For the MSI group, exercise may be appropriate for muscle balance and controlling excessive movement.
Our findings showed improved physical function in both groups. FMS is positively related to core strength.23 Tasks of FMS need individual abilities, requiring a combination in physical activity. Five tasks in FMS require trunk stability. Also, back endurance plays a very important role in spinal stability during prolonged physical activity. MSI and general exercise may provide trunk stability. However, the MSI group showed a larger difference in the mean difference. Noh et al.11 and Park et al.12 suggested that minimizing the method of unwanted lumbopelvic rotation increased the activation of abdominal muscles better than conventional methods while maintaining active straight leg raising. These results in the MSI group would be due to restricted excessive lumbopelvic motion by isometric trunk muscles during movement of the upper or/and lower extremities. Pre-intervention FMS scores of our subjects with NCLBP and pre-intervention FMS scores were approximately 10 points. If football players’ scores were 14 or less for FMS performance,24 this predicted their injury. After the six-week intervention in the MSI group, FMS scores averaged 13.83. Although the MSI group’s post-intervention score was less than 14, this result is clinically meaningful because of subjects with NCLBP in our study.
The present study found that the self-report questionnaires for psychosocial problems and disability improved in both groups, but there was no significant difference between the groups. In the systemic reviews, exercise therapy slightly reduced sick leave during the first year and decreased the proportion of patients who had not returned to work at 1 year.19 Brox et al. reported that cognitive intervention and exercise therapy were effective in the FABQ of patients with NCLBP.25 Our results showed that there were effective psychosocial problems and disability in both groups in NCLBP. A corrective exercise in MSI exercise is a method restraining excessive motion of the lumbar spine to a specific direction that elicits or increases symptoms. Such exercise was suggested to reduce the fear of physical activities in the subgroup by MSI classification.
This study had some limitations. First, our study had a six-week exercise intervention, and we immediately measured the outcome after the intervention. NCLBP has a high recurrence rate. Future studies should investigate a longer exercise period and a long-term follow-up. Thus, these results cannot be generalized to patients with NCLBP because the sample size was small.
CONCLUSIONS
The study compared the effects of specific exercise in the subgroups by classification and general exercises in patients with NCLBP. Our findings showed that the VAS score decreased and the Sorensen test and FMS increased post-intervention within the MSI group. The mean difference in the VAS, the Sorensen test, and FMS scores were significantly greater in the MSI group than in the general group. Therefore, a specific intervention based on MSI, applied to a homogenous group of NCLBP patients, may provide appropriate therapeutic exercises in the clinical setting.







