INTRODUCTION
Hallux valgus (HV) is a progressive foot deformity characterized by lateral deviation of the first metatarsal creating an apex (a deformity) at the first metatarsal-phalangeal joint, with or without medial soft tissue enlargement of the first metatarsal head (bunion).1,2,3 The prevalence of HV ranges from 12 to 70% in the general population.4,5 Nix et al. (2010) reported pooled prevalence estimates for HV of 23% in adults aged 18–65 years and 35.7% in those aged>65 years.6 HV may cause several health problems, changing the foot balance, triggering laxity of the static stabilizers (in turn disrupting muscle balance), and increasing the risk of falling.4,7,8
The metacarpophalangeal joint is dynamic, being affected by many muscles, joints, and ligaments.1,2Most previous studies on HV focused on the possible relationship between the deformity and muscles and/or ligaments of the foot and lower leg.2,3 Recent studies used kinematic chain theory to link HV with the lower limb joints and bones.9,10 The theory suggests that movement at one joint of a lower extremity may affect all other joints via a chain reaction.2,3,9,10 A literature search for causes of HV did not produce any data on the general population.1,2,3Also, no study has yet compared lower leg alignment and muscle flexibility between two sides in subjects with asymmetric HV angles (HVAs). We assessed iliotibial band flexibility and tibial torsion angle in subjects with asymmetric HVAs. We hypothesized that both parameters would differ between the legs.
METHODS
A pilot test was initially performed to determine the required sample size. A sample size was calculated based on a two-group t-test in G*Power software package (version 3.1.9.2; Franz Faul, University Kiel, Germany). The power analysis used data on HVAs. A total of 14 subjects were required for a power of 80% (α=0.05, d=0.98). We recruited 15 subjects with differences>5° in the HVA between the two legs (5 males and 10 females). The mean age was 33.0±10.3 years, mean height 166.5±6.1 cm, and mean weight 61.2± 9.2 kg. The investigators had 14 and 6 years of physiotherapy experience, respectively. The exclusion criteria were radiating pain, strain of any lower extremity muscle, and any joint contracture. Prior to the study, the principal investigator explained all procedures and all subjects signed informed consent forms.
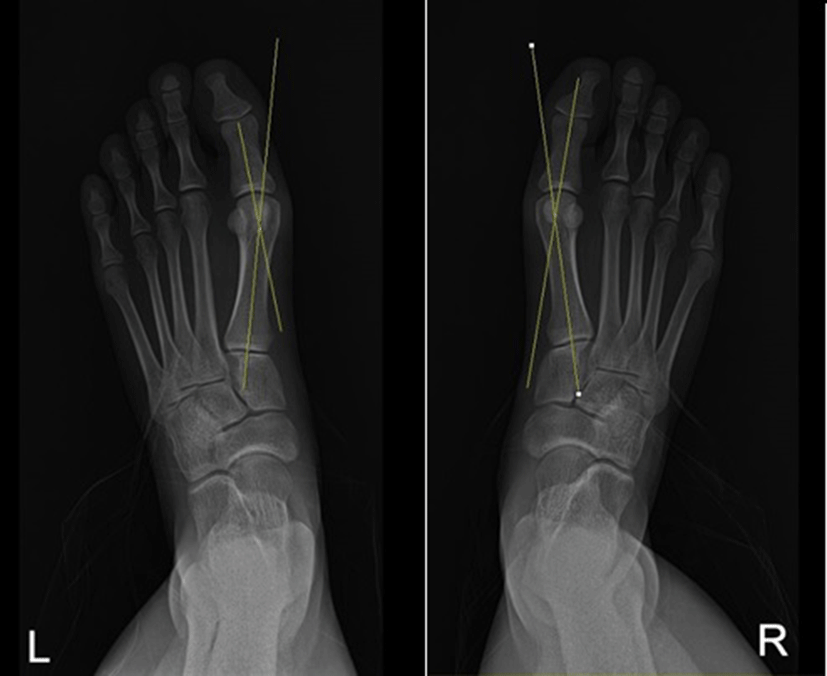
The HVA was measured on radiographs at the intersection between the long axis of the first metatarsal and the proximal phalanx.1,2,3,5 The axis of the first metatarsal was drawn through points that proximally and distally bisected the shaft of the bone, and the axis of the proximal phalanx was drawn through the midpoints of the proximal and articular surfaces (Figure 1).1,2 Three measurements were made and the average was used in analysis.
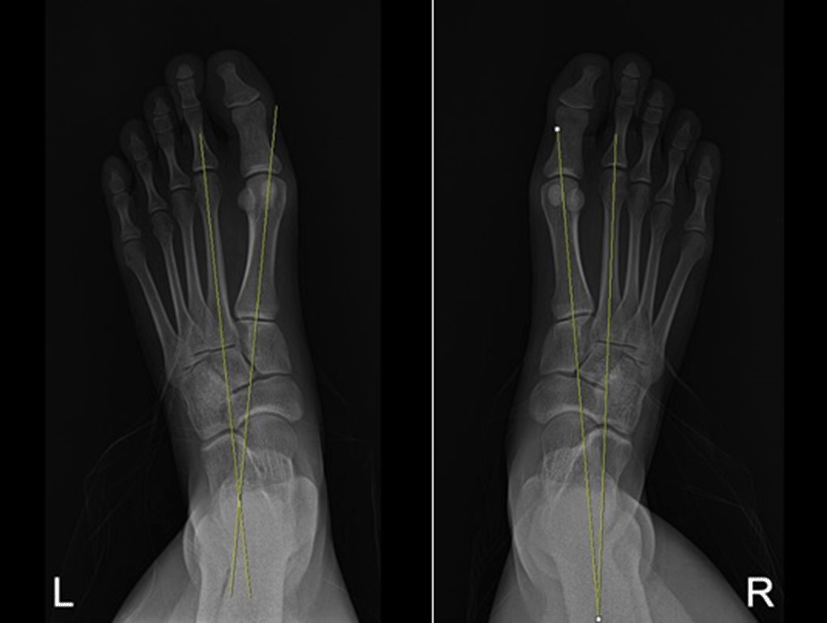
The intermetatarsal angle was measured between the long axes of the first and second metatarsals (Figure 2).1,2,3,5 Three measurements were made and the average was used in analysis.
Each participant bent the knee through 90° and held the ankle in the neutral prone position. The examiner located the middle of the medial and lateral malleolus (in the anterior-posterior direction) at the level of the ankle, and marked the midpoint with a pen.11 To derive the axis passing through both malleoli, a line connecting the points of the medial and lateral bones was drawn on the sole of the heel. The stationary and movable arms of the goniometer was placed in line with this axis and on the longitudinal axis of the femur, respectively (Figure 3).11 The examiner recorded the angle between the two lines as the tibial torsion angle.11Each participant was instructed to remain relaxed during measurement to minimize rotation of the lower limb. Three measurements were made and the average was used in analysis.
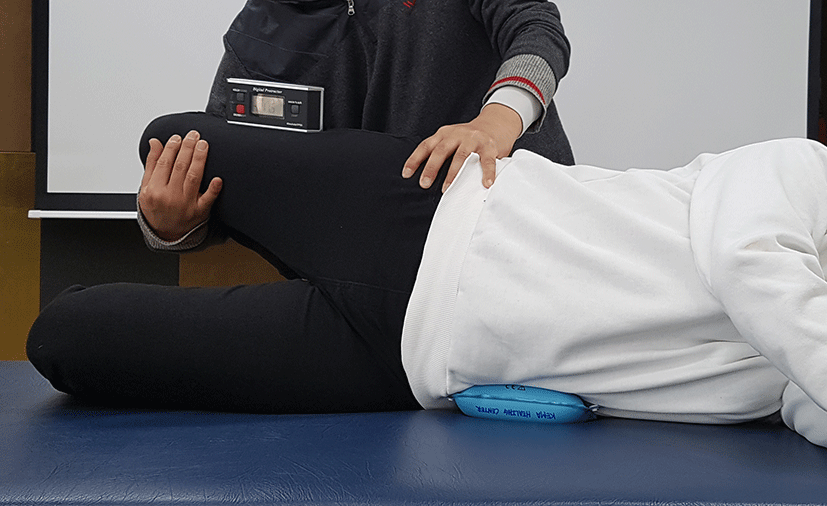
We used the Ober test to assess iliotibial band flexibility.12 Each participant was instructed to bend the lower leg through 90° to maintain the spine in a neutral position while lying on the side (Figure 4). The examiner stood behind the participant and placed a stabilizing hand on the upper iliac crest. The hip joint of the upper leg was placed in abduction and extension and the knee joint flexed through 90°. The examiner recorded the adduction angle with the upper leg pointing to the floor to a certain extent, ensuring that the pelvis did not move. Three measurements were made and the average used in analysis.
Using anterior and posterior radiographs, obtained by employing the same protocol in the same hospital, the first examiner measured the HVA and intermetatarsal angle. The second examiner measured the tibial torsion angle and iliotibial band flexibility while blinded to the leg with the greater HVA. The first examiner collected all data and performed all analyses.
We used the independent t-test to compare differences in the HV, intermetatarsal, and tibial torsion angles, and in iliotibial band flexibility, between the two sides. The level of statistical significance was set to 0.05. SPSS software (ver. 12.0; SPSS, Inc., Chicago, IL, USA) was employed for all statistical analyses.
RESULTS
The HV and intermetatarsal angles differed significantly between the two sides (both p<0.05). Iliotibial band flexibility was significantly lower on the side with the greater HVA (p<0.05). The tibial torsion angle did not differ significantly between the two sides (p>0.05).
DISCUSSION
Earlier studies explored whether lower extremity alignment affected HV.2,13,14 We sought a link between asymmetric HVAs and lower extremity alignment. Iliotibial band flexibility differed significantly between the two sides. The causes of HV vary widely.2,6,15Yamada et al. (2014) reported that a patient with a valgus deformity of the hindfoot also exhibited an HV deformity, and suggested that correction of any severe valgus, the calcaneal lateral offset, and any pronated foot deformity was required for HV rehabilitation.15 Foot pronation is caused by malfunction of muscles connected to the adjacent joint, and is closely associated with both adduction of the hip joint and internal rotation of the knee joint.16,17,18Previous studies reported that these movements of proximal segments which is associated with excessive foot pronation was caused by predominance of tensor fascia lata during walking or stair-climbing.17,18 Then, although the amount of foot pronation was not measured in this study, it can be expected that asymmetric foot pronation may effect on the difference of iliotibial band flexibility in subjects with asymmetric HVAs.
In this study, the tibial torsion angles differed somewhat between the two sides but the difference was not significant, possibly because of the low numbers of subjects. We conducted a power analysis to determine the proper sample size before the study. Although the sample size was determined by 14, it was required 25 subjects to explore a possible difference in the tibial torsion angle, when performing the power analysis with results of this study. If we increase the number of subjects, there is a risk of increasing "type 1 errors". Therefore, current study is proper in number of subjects. Thus, we suggest that asymmetry of HVA influences more IT band flexibility than tibial torsion angle.
Our study had several limitations. First, this was a static study; we do not know whether dynamic status differed and, if so, how. The body forms a connected mechanical chain.2,3,13,16 HV causes not only foot problems, but also general malalignment and muscle strength imbalance in the lower extremities.2,3,4 The entire exercise chain requires study, i.e., not only the knee joint, but also the hip. Second, because subjects with normal as well as mild HVA participated in this study, the results of this study cannot be generalized in clinical setting for HV rehabilitation. Our inclusion criterion was a between-foot difference≥5°. Previous studies classified HV into three types by the HVA and intermetatarsal angle: normal (HVA<15°, intermetatarsal angle<9°) mild (HVA 15-20°, intermetatarsal angle 10-15°), moderate (HVA 21-40°, intermetatarsal angle 15-20°), and severe (HVA>40°, intermetatarsal angle>20°).19,20 The HVAs of the feet of our subjects were 17.63±5.75° and 12.40±4.89°, respectively. The intermetatarsal angles were 12.37±2.68° and 9.87±2.45°, respectively. To generalize in clinical setting for HV rehabilitation, further work is required to determine whether iliotibial band flexibility and tibial torsion differ among subjects normal and with HV groups in three stages.
CONCLUSION
Subjects with asymmetric HVAs exhibited asymmetric knee joint musculoskeletal elements. Each lower extremity forms a kinematic chain, and any abnormal joint alignment triggers misalignment and asymmetry of adjacent joints and muscles. Therefore, we suggest that iliotibial band flexibili-ty should be considered in HV rehabilitation.