INTRODUCTION
Normal thoracic alignment of the thoracic spine is a flexion curve of 40° with mild posterior convexity and an even distribution of flexion.1 From the plumb line, the center of gravity lies in front of the thoracic spine and flexes the thoracic spine.2 The thoracic spine extensors play a major role in maintaining upright posture for optimal spinal balance.3
An increase in the thoracic kyphotic angle may alter physiologic loading in the spine as a consequence of a shift in trunk mass, leading to increased flexion moments and compression and shear force imposed on the spinal segment.4In addition, trunk extensor muscle weakness can result from reduced muscle activity due to posture changes, arm length moments, force vector orientation, or an altered length-tension relationship within overstretched trunk extensor muscles.5,6
To correct excessive thoracic kyphosis (flexed thoracic spine) and strengthen the thoracic extensor muscles, prone thoracic extensor strengthening is widely used in clinical settings.1,8 During prone thoracic extensor strengthening, excessive compensation in nearby joint segments (lumbar spine extension) may be less effective for extending the thoracic spine and produce lumbar spine pain due to excessive compressive force and shearing force.5,8
Although selective strengthening of the thoracic extensor muscle is recommended for therapy and training, limited information is available to help clinicians design an effective strengthening program. We investigated the most effective exercise for strengthening the thoracic spine extensors. We compared trunk muscle activity in three thoracic extensor strengthening exercises: active prone thoracic extension (APTE), active prone thoracic hyper-extension (APHE), and active sitting thoracic extension (ASTE). We hypothesized that the ASTE exercise would selectively strengthen the thoracic extensor muscles.
METHODS
The participants in this study were 16 volunteers (12 male, 4 female; mean age: 23.2±1.7 years old; height: 173.1±6.6 cm; weight: 70.4±10.3 kg). Participants were included if they had no history of thoracic pain or injuries, and were able to maintain 5 s test positions. The subjects reported no pain during the test procedure. Informed consent was obtained from all subjects.
A surface electromyography (EMG) system (TeleMyo DTS, Noraxon, Scottsdale, AZ, USA) was used to analyze the activity of the longissimus thoracis (LT), iliocostalis thoracis (ICT), and iliocostalis lumborum (ICL) using analysis software. Filtered movement artifacts were eliminated using a 20-450 Hz digital band-pass filter (Lancosh FIR). The sample rate was set to 1,024 Hz. The root mean square was used to process EMG signals with a moving window of 50 ms. EMG signals were recorded for 5 s (2-4 s used for data analysis). Two surface electrodes with an inter-electrode distance of 2 cm were positioned on the LT, ICT, and ICL. Two electrodes were placed in the middle of each muscle belly and parallel to the muscle fibers. The electrode sites were shaved and rubbing alcohol was used to reduce skin impedance. For LT recordings, the electrodes were placed at the T10 level, midway between a line through the spinous process and a vertical line through the posterior superior iliac spine, approximately 5 cm laterally. For ICT recordings, the electrodes were placed at the T10 level, midway between the lateral palpable border of the erector spinae and a vertical line through the posterior superior iliac spine. For ICL recordings, the electrodes were placed at the L3 level, midway between the lateral palpable border of the erector spinae and a vertical line through the posterior superior iliac spine.10 The maximum voluntary isometric contraction (MVIC) of the LT, ICT, and ICL was used for normalization. To measure the MVIC, the subjects lay in a prone position and placed their hands on their head with their legs strapped to the table.10Trunk extension was performed with maximum isometric effort against the examiner’s resistance. Muscle contraction was held for 5 s with maximal effort. The first and last seconds of each MVIC trial were discarded, and the remaining 3 s of EMG data were used in the analysis. This procedure was repeated three times, with a 30 s rest period between sessions. The data for each trial were expressed as a percentage of the calculated mean root mean square (RMS) of the MVIC (%MVIC), and the mean %MVIC of the three trials was used in subsequent analyses.
APTE was performed with the xiphoid process aligned with the table edge and the subjects’ arms crossed at the chest. The subjects were asked to raise their trunk to horizontal (parallel to the ground) and maintain this position for 5 s using a target bar.10 APTH was performed with the xiphoid process aligned with the table edge and the subjects’ arms crossed at the chest. The subjects were asked to hyperextend their trunk by 7 cm at the level of T8 and maintain this position for 5 s using a target bar.10 ASTE was performed with the participants sitting on a chair with their arms supported on the table. This exercise was performed in sequential steps. First, the participants were asked to slump the back into thoracic and lumbar flexion. Second, while this position was held, the participants were asked to actively extend only the thoracic spine with the arms supported on the table and the xiphoid process supported on the edge of table. The participants maintained this position for 5 s. Familiarization with each exercise was performed during a 10 min period before data collection (Figure 1).
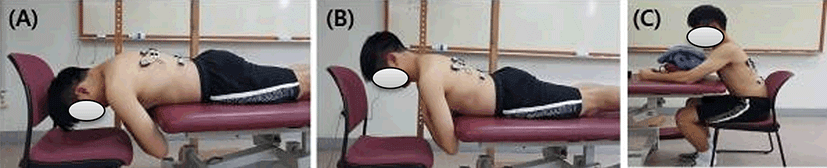
EMG data were collected while the participants maintained the test position without loss of balance and without trunk rotation. We collected EMG data during the middle 3 s of the 5 s period. The average of each set of three trials was used for data analysis. Each participant completed each exercise three times with 1 min of rest between exercises.
We used the SPSS Statistical Package for Windows (version 23.0; IBM SPSS, Armonk, NY) for data analysis. The data are expressed as means±standard deviations. We performed the Kolmogorov-Smirnov Z-test to assess whether continuous data approximated a normal distribution. A one-way analysis of variance (ANOVA) with repeated measures was used with a P level of 0.05. When a significant difference was detected, we used the Bonferroni adjustment (Padj) with a P level of 0.017 (i.e., 0.5/3).
RESULTS
All continuous variables were found to approximate a normal distribution (Kolmogorov-Smirnov Z-test, p>0.05). The normalized EMG activities of the ICT, ICL, and LT muscles are shown in Table 1. The ICT, ICL, and LT muscle activities were significantly different among exercises (p< 0.05) (Figure 2). We observed the largest increase in ICT, ICL, and LT muscle activity during APTH and the least muscle activity during ASTE. By contrast, the ICT/ICL and LT/ICL composition ratios were greatest during ASTE compared to other exercises (p<0.05) (Figure 2).
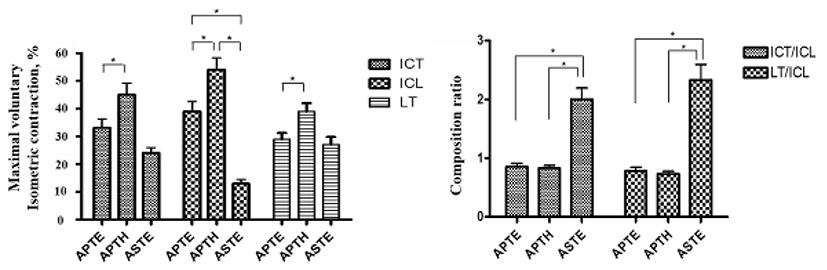
DISCUSSION
Trunk extension strengthening (TES) exercises are useful for strengthening the erector spinae to improve trunk exten- sion or prevent the natural progression of kyphosis.8 However, general TES exercises can lead to greater (excessive) degrees of lumbar extension than thoracic extension.11 The current trend in exercise programs is to focus on functional restoration by strengthening specific target muscles with minimal participation of the surrounding musculature.12 Hence, we investigated the most effective of three TES exercised to selectively stimulate thoracic extensor muscle (ICT and LT) activity while minimizing the use of the lumbar extensor (ICL).
We compared the EMG activity of trunk extensor muscles during three different TES exercises. APTH led to greater EMG activity levels than the other exercises. However, ASTE caused selective activation of the thoracic extensor muscles (ICT, and LT). There are two possible explanations for these results. First, trunk extensor muscle (ICT, LT, and ICL) activity is related to the trunk extension angle. The joint angle is influenced the activation level of the muscle.13 ICT, LT, and ICL muscle activity was greater in APTH than in APTE and ASTE. Although we did not directly measure kinematic data to determine the thoracic spine extension angle, APTH was performed in a more extended position (trunk hyperextended by 7 cm at the level of T8) compared to the other exercises (neutral position maintained). Inappropriate or excessive lumbar extension by ICL produces pain due to greater disk loading, compressive force, and shearing force caused by an increased spinal curve in the sagittal plane.5,9 For safe and effective TES exercise, it is necessary to minimize lumbar extensor muscle (ICL) activity to decrease the stress on the lumbar spine during exercise. Second, the synergistic activity of the erector spinae pars thoracis (ICL and LT) and lumborum (ICL) muscle is assumed to be the main mechanism of trunk extension; these muscles do not form a homogeneous muscle mass, but rather have anatomical and functional differences.10 Our findings demonstrated that ASTE was the most effective exercise to selectively activate the thoracic extensor muscles (ICT and LT) while minimizing the lumbar extensor muscle (ICL).
Our study had several limitations. First, our results are not widely generalizable because all participants were healthy students. Thus, additional research is needed to establish whether our findings apply to participants with thoracic kyphosis or thoracic flexion syndrome. Second, we did not obtain kinematic measurements of spine movements; further study is required for their assessment. Third, our study was cross-sectional, such that longitudinal follow-up is warranted to determine the long-term effects of selective training for patients who have thoracic kyphosis or thoracic flexion syndrome.
CONCLUSIONS
We investigated the EMG activity of the trunk extensor muscles (ICT, LT, and ICL) during three TES exercises. Our findings showed that selective activation (relative ratio of thoracic to lumbar erector spinae muscles) was significantly greater in ASTE than in APTE and APTH. These findings suggest that ASTE exercise is beneficial for selective thoracic spine extensor strengthening, minimizing excessive lumbar spine extensor activation.







